

The herpes simplex virus (HSV) causes blisters and sores often around the mouth, nose, genitals, and buttocks, but they can occur almost anywhere on the skin. HSV infections can be very annoying because they may reappear periodically. The sores may be painful and unsightly. For chronically ill people and newborn babies, the viral infection can be serious, but rarely fatal. There are two types of HSV - Type 1 and Type 2.
Often referred to as fever blisters or cold sores, infections are tiny, itchy, clear, fluid-filled blisters, often grouped together. They most often occur on the face.
Cold sores are caused by certain strains of the herpes simplex virus (HSV). HSV-1 usually causes cold sores. HSV-2 is usually responsible for genital herpes. But either type can spread to the face or genitals through close contact, such as kissing or oral sex. Shared eating utensils, razors and towels might also spread HSV-1.
Cold sores are contagious even if you don't see the sores. Cold sores spread from person to person by close contact, such as kissing.
There are two kinds of infections - primary and recurrent. Although most people get infected when exposed to the virus, only 10 percent will actually develop sores. The sores of a primary infection appear two to twenty days after contact with an infected person and can last from seven to ten days.
The number of blisters varies from a single to a group of blisters. Before the blisters appear, the skin may itch, sting, burn, or tingle. The blisters can break as a result of minor injury, allowing the fluid inside the blisters to ooze, crust & scab. Eventually, crusts fall off, leaving slightly red, healing skin.
The sores from the primary infection heal completely and rarely leave a scar. However, the virus that caused the infection remains in the body. It moves to nerve cells where it remains in a resting state.
People may then have a recurrence either in the same location as the first infection or in a nearby site. The infection may recur every few weeks or not at all.
Children under 5 years old may have cold sores inside their mouths and the lesions are commonly mistaken for canker sores. Canker sores involve only the mucous membrane and aren't caused by the herpes simplex virus.
Recurrent infections tend to be mild. They can be set off by a variety of factors including fever, sun exposure, a menstrual period, trauma (including surgery), or nothing at all.
Cold sores generally clear up without treatment. See your doctor if:
There's no cure for cold sores, but treatment can help manage outbreaks. Prescription antiviral pills or creams can help sores heal more quickly. And they may reduce the frequency, length and severity of future outbreaks.
Link to Domeboro instruction sheet
Hemangiomas/Angiomas are growths of blood vessels and other red spots which can be dilated blood vessels that take the form of a birthmark (Nevus Flameus).
Hemangiomas is a bright red birthmark that shows up at birth or in the first or second week of life. It looks like a rubbery bump and is made up of extra blood vessels in the skin. A hemangioma can occur anywhere on the body, but most commonly appears on the face, scalp, chest or back. It can grow out of proportion to the child for the first 8 months of life before the growth rate levels off. Therefore, it is important to evaluate these growths early especially if they are located around the eyes, mouth, genitals, scalp, neck or anus. Many hemangiomas disappear by age 5, and most are gone by age 10. The skin may be slightly discolored or raised after the hemangioma goes away.
Red bumps that we acquire with age or genetics are referred to as cherry angiomas. They often arise later in life and while not dangerous, can be considered unsightly. Their treatment can be simple and often requires no wound care enabling one to return to daily activities immediately.
A doctor can usually diagnose a hemangioma just by looking at it. Tests usually aren't needed.
A hemangioma is made up of extra blood vessels that group together into a dense clump. What causes the vessels to clump isn't known.
Hemangiomas occur more often in babies who are female, white and born prematurely.
Occasionally, a hemangioma can break down and develop a sore. This can lead to pain, bleeding, scarring or infection. Depending on where the hemangioma is situated, it may interfere with your child's vision, breathing, hearing or elimination, but this is rare.
Treating hemangiomas usually isn't necessary because they go away on their own with time. But if a hemangioma affects vision or causes other problems, treatments include medications or laser surgery:
If you're considering treatment for your child's hemangioma, weigh the pros and cons with your child's doctor. Consider that most infantile hemangiomas disappear on their own during childhood and that treatments have potential side effects.
Hand Eczema is dry skin of the hands. It is more common in the winter when the air holds less moisture and the cold wind increases water loss from the skin. It is worsened by frequent hand washing, using harsh soaps, not using moisturizer, and not using cotton-lined rubber gloves when doing work with detergents.
Genital warts affect the moist tissues of the genital area. They can look like small, flesh-colored and be flat or bumpy or have a cauliflower-like appearance. Some genital warts are so small they cannot be seen. They can cause pain, discomfort or itching. Genital warts, also known as venereal warts, or condylomata acuminata, are caused by the human papilloma virus (HPV). More than 100 types of HPV are known to exist. Low risk types (HPV 1, 2, and 3) cause warts on the hands, feet, and other parts of the body. The low risk strains - Types (6 and 11) can cause warts on the genitals or anus (genital warts), and other high risk strains - Types (HPV 16 and 18) can cause cancer of the cervix, external genitalia, vulva, and anus.
Genital warts are sexually transmitted disease (STD) and all partners should be checked thoroughly. They can also be seen in infants who have been delivered vaginally to mothers with HPV in their genital tracts; therefore, alternate methods of delivery should be considered.
Only a small percentage of people infected with HPV will develop genital warts. Many people are carriers of HPV who may never develop warts, but may still be able to pass HPV to their sexual partners. The incubation period from contracting HPV until the development of warts may be several months although some people may not develop warts for years after contact with HPV. People who have lower immunity due to cancer, AIDS, organ transplantation, immune suppressive medications, or certain other medications are more susceptible.
To diagnose this condition, your doctor will do the following:
Although HPV isn't curable in all cases, genital warts are treatable. You can also go extended periods of time without an outbreak, but it may not be possible to get rid of the warts forever. That's because genital warts are only a symptom of HPV, which may become a chronic, lifelong infection for some.
If you've developed genital warts, your doctor has a few options for treatment. The fastest way to remove them is through surgery or to freeze them off with liquid nitrogen. Some doctors might use an electric current or laser treatment to burn off the warts.
Genital warts can go away with treatment from your healthcare provider or with prescription medicine. If left untreated, genital warts may go away, stay the same, or grow in size or number. Cervical precancer treatment is available.
Your doctor may apply a mild acidic solution, called an acetowhite test, to your skin to help make genital warts more visible. It may cause a slight burning sensation.
If you have a vulva, your doctor may also need to perform a pelvic examination, because genital warts can occur deep inside your body.
While visible genital warts often go away with time, HPV itself can linger in your skin cells. This means you may have several outbreaks over the course of your life.
So managing symptoms is important because you want to avoid transmitting the virus to others. That said, genital warts can be passed on to others even when there are no visible warts or other symptoms.
You may wish to treat genital warts to relieve painful symptoms or to minimize their appearance. However, you can’t treat genital warts with over-the-counter (OTC) wart removers or treatments.
Your doctor may prescribe topical wart treatments that might include:
If visible warts don’t go away with time, you may need minor surgery to remove them. Your doctor can also remove warts through these procedures:
To help prevent genital warts, HPV vaccines, condoms, and other barrier methods are available:
If you think you have genital warts, talk with your doctor. They can determine if you have warts and what your best treatment options are.
In addition, it’s important to talk with your sexual partner. This may sound difficult, but being open about your condition can help you protect your partner from also getting an HPV infection and genital warts.
Genital warts are a complication of a low risk HPV infection that’s common and treatable. They can disappear over time, but treatment is essential in preventing their return and possible complications.
Eczema is a a type of dermatitis. The terms "eczema" and "dermatitis" are a group of skin conditions that cause skin inflammation and dry, itchy patches of skin. It’s a common condition that isn’t contagious. Symptoms of eczema can flare up if you contact an irritant or an allergen. There are treatments available to help you manage symptoms, but there isn’t a cure.
It’s possible to have more than one type of eczema at the same time.
Eczema can affect anyone at any age. Symptoms usually appear during childhood and last into adulthood. You might be more at risk of having eczema if you have a family history or a diagnosis of:
Eczema is common and affects more than 31 million Americans. Infants are prone to eczema, and 10% to 20% will have it. However, nearly half of all infants diagnosed with eczema outgrow the condition or have significant improvement as they get older.
Eczema doesn’t usually cause pain. If you scratch your skin, you could break the surface of your skin and create a sore, which could be painful. Some types of eczema, like contact dermatitis, cause a burning sensation and discomfort.
Eczema can look different on each person diagnosed with the condition. If you have a dark skin tone, an eczema rash can be purple, brown or gray. If you have a light skin tone, an eczema rash can look pink, red or purple.
While eczema can cause your immune system to overreact, it isn’t classified as an autoimmune condition. Research is ongoing to learn more about how eczema interacts with your immune system.
Q. Since this condition is associated with allergies, can certain foods be the cause?
A. Rarely (perhaps 10%). Although some foods may provoke atopic dermatitis, especially in infants and young children with asthma, eliminating those foods is rarely a cure. You should eliminate any foods that cause immediate severe reactions or welts.
Q. Are environmental causes important and should they be eliminated?
A. Rarely. The elimination of contact or airborne substances does not bring lasting relief. Occasionally, dust and dust-catching objects like feather pillows, down comforters, kapok pillows and mattresses, cat and dog dander, carpeting, drapes, some toys, wool, and other rough fabrics, can worsen atopic dermatitis.
Q. Are skin tests, like those given for hay fever or asthma, of any value in finding the causes?
A. Sometimes, but not as a rule. A positive test means allergy only about 20% of the time. If negative, the test is good evidence against allergy.
Q. Are shots (immunotherapy injections) such as those given for hay fever and other allergies useful?
A. Not usually. They may even make the skin condition worse in some patients.
Q. What should be done to treat this condition?
A. We will provide advice on avoiding irritating factors in creams and lotions; rough, scratchy, or tight clothing; and woolens. Rapid changes of temperature and any activity that causes sweating can aggravate atopic dermatitis. Proper bathing, moisturizing, and dealing with emotional upsets which may make the condition worse should be discussed.
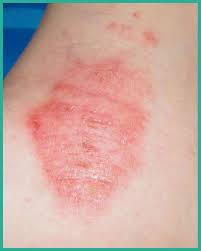
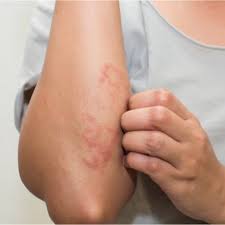
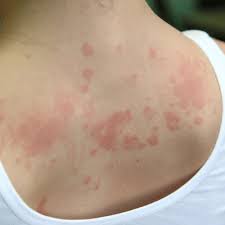
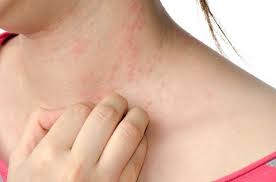
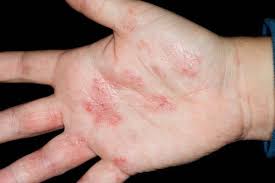
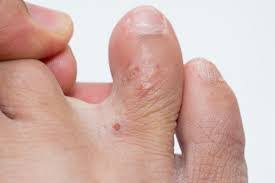
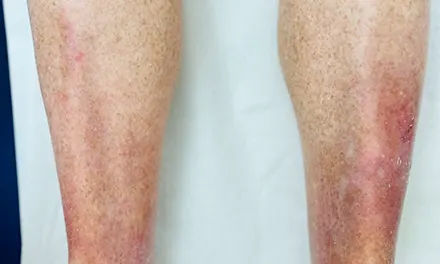
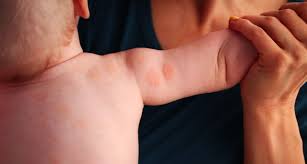
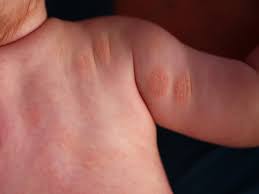
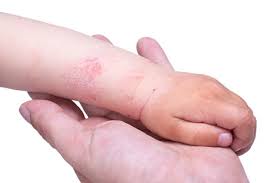
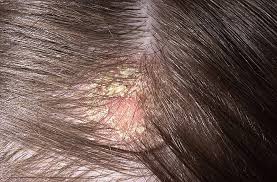
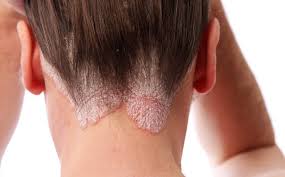
Dry skin (eczema) and Keratosis Pilaris, are common disorders of the skin. Keratosis Pilaris (KP) is characterized by rough epidermal regions and patches of small acne-like bumps that typically appear on the upper arms, thighs, buttocks, and cheeks. Doctors typically identify KP in patients who complain of the appearance of “gooseflesh,” “goose bumps,” or “chicken skin” on various body parts. These bumps can be white, tan, or red in color. The condition is caused by the keratinization (or cellular “hardening”) of the skin’s hair follicles.Keratosis Pilaris often runs in families. Although its poses no serious medical threat, KP is often considered cosmetically displeasing. During particularly violent outbreaks, many KP sufferers report persistent itching in the affected area. The disorder can affect people of all ages, but most patients find that the major symptoms of KP disappear completely by age 30.
Because the general public is unaware of KP as a medical condition, many individuals are diagnosed with the condition when visiting dermatologists and other medical professionals for unrelated skin conditions. KP is often seen in patients with other epidermal disorders such as dry skin and eczema. If moisturizing doesn't help make an appointment as prescription strength treatment may be needed.
A cyst is a closed sac with a defined membrane and division on the nearby tissue.
Cysts may contain fluid, air or semisolid material. Parasites — such as trichinosis, dog tapeworm and echinococcus. Cysts are typically benign growths that consist of a wall that makes the contents. Often these bumps are cosmetically unacceptable or patients desire removal in the event they may rupture. Although cysts can remain intact for a lifetime, may go away on their own.There is also the risk of rupturing, which can lead to a great deal of inflammation, pain and infection. This necessitates surgical excision.
Sebaceous / Epidermoid Cysts are typically a common, noncancerous type of cyst. Sebaceous cysts arise from sebaceous glands that secrete oily matter that lubricates the hair and skin. These cysts, which may be hereditary, are caused when glands or hair follicles become blocked. Trauma to the skin is another likely cause of a cyst. These cysts appear as small bumps beneath the skin. Although they can occur almost anywhere on the body, they typically appear on the face, neck and trunk. A foul odor may be secreted from the outside skin of the cyst. Sebaceous cysts grow slowly and usually are not painful; thus, treatment is rarely needed. However, options are available if these cysts become painful or have an unacceptable appearance.
There are three common cyst removal techniques specifically for sebaceous cysts — conventional wide excision, minimal excision and punch biopsy excision.
Lastly, these cysts typically appear on the scalp which originate in the skin and hair follicles, may cause lumps under the skin, but often do not require surgical removal.
"OUCH! What Bit Me?"
Sometimes it’s easy to tell what bit you: maybe you reach down to swat at the bug and catch a glimpse of it. Sometimes though, it’s harder to tell. You might not notice the bite as it’s happening. Instead you don’t even realize you’ve been bitten until the spot starts to itch.
Although most bug bites and stings are harmless, some can be dangerous. This is especially true if you are allergic to the bug’s venom, or if the bug is carrying a disease. Most bug bites and stings can be safely treated at home with topical medication. However, sometimes a bug bite or sting could turn into something serious – particularly if you have been bitten or stung by many insects at the same time.
In the United States, it’s common to experience a bite or sting from the following types of bugs:
When weather permits, wear long sleeves and pants. They can add an extra layer of protection between you and your exposed skin. Light-colored clothing makes ticks easier to spot. Do a quick clothing and body check for ticks once you get inside.
Remember, insect repellants are your friend. The best ones contain DEET, like DEEP Woods OFF or ones that contain picaridin. Be sure to use any insect repellants according to the directions on the label.
For insect bites and stings that itch, you can put an ice pack on the spot and/or use an over-the-counter itch cream; for example, hydrocortisone. You may choose to instead take an oral antihistamine. Ice packs can also reduce swelling.
It’s important to pay attention to your symptoms. If you feel tired all the time, you have a headache, fever or body aches, or you develop a rash after a bug bite, see a board-certified dermatologist immediately.
Go to the emergency room immediately if you experience any of the following symptoms after a bug bite or sting:
Age spots are small, flat dark areas on the skin. They vary in size and usually appear on areas exposed to the sun, such as the face, hands, shoulders and arms. Age spots are also called sunspots, liver spots and solar lentigines.
Age spots can look like cancerous growths. True age spots don't need treatment, but they are a sign the skin has received a lot of sun exposure and are an attempt by your skin to protect itself from more sun damage. You can help prevent age spots by regularly using sunscreen and avoiding the sun.
Age spots may affect people of all skin types, but they're more common in adults with light skin. Unlike freckles, which are common in children and fade with no sun exposure, age spots don't fade.
Age spots don't require medical care. Have your doctor look at spots that are black or have changed in appearance. These changes can be signs of melanoma, a serious form of skin cancer.
It's best to have any new skin changes evaluated by a doctor, especially if a spot:
Age spots are caused by overactive pigment cells. Ultraviolet (UV) light speeds up the production of melanin, a natural pigment that gives skin its color. On skin that has had years of sun exposure, age spots appear when melanin becomes clumped or is produced in high concentrations. Also, the use of commercial tanning lamps and beds can cause age spots.
We offer a range of advanced laser therapies tailored to the type and depth of discoloration, whether you’re dealing with brown spots, melasma, sun damage, or red marks from acne or rosacea. Each treatment is selected based on your unique skin tone, condition, and goals.
Lasers for Brown Spots, Melasma & Sun Damage:
These lasers use ultra-short pulses to break up unwanted pigment while minimizing damage to surrounding skin, ideal for darker skin tones.
Q-switched Nd:YAG Laser: Targets deep pigmentation, including melasma and post-inflammatory hyperpigmentation (PIH), with precision and safety for all skin tones.
Fractional Lasers: These versatile lasers treat pigmentation and improve overall skin quality by stimulating collagen production and resurfacing the skin. Great for: PIH (post inflammatory hyperpigmentation), sun damage, acne scarring, uneven tone, and texture.
Vascular Lasers:
Specialized for redness and pink-toned PIH (post inflammatory hyperpigmentation), especially from acne or rosacea.
Vbeam (Pulsed Dye Laser):
Targets blood vessels to reduce red marks, flushing, and inflammation. A gentle, effective option for sensitive or reactive skin types.
Each laser treatment is customized to your skin’s needs to ensure safe, effective results. During your consultation, we’ll determine the best approach—often combining laser therapy with topical treatments to maximize improvement and minimize recurrence.
For brown marks on deeper skin tones, we use a combination of hydroquinone, kojic acid, Vitamin C, and AHAs to gently and effectively lighten dark spots while brightening and smoothing the skin.
These clinically proven ingredients work synergistically to visibly brighten, lighten, and tighten the skin, revealing a more even, radiant complexion.
JAS Anti - Aging TRIO, expertly formulated to replenish, exfoliate, and restore your skin’s natural glow.
To help avoid age spots and new spots after treatment, follow these tips for limiting your sun exposure:
⚠️ Important
Always see a board-certified dermatologist or laser specialist, especially if you have darker skin.
Sun protection is non-negotiable—exposure after treatment can trigger new pigment.
If you are tired of looking older or want the spots removed, schedule a laser consultation and restore your skin to its natural beauty. Our Cosmetic Consultation Reimbursement policy is offered to all patients. Schedule an office visit to discuss your concerns and skincare goals with Dr. Robinson and the office visit cost will be applied to the future cost for the "consulted procedure". The "consulted procedure" must be completed within 30 days of your consult visit.
Birthmarks are abnormalities of the skin that are present when a baby is born.
A birthmark can be red or brown.
A red or vascular birthmark is made up of dilated blood vessels. Two types are hemangiomas and port-wine stains. Although they can resolve spontaneously on their own, some can cause deformities and become more purple in color. With the advent of laser treatment, the Nevus Flameus can be cleared and subsequent deformities prevented.
A Nevus of Ota, Nevus of Ito and Mongolian spot are brown to bluish birthmarks that usually occur around the eye, shoulder and trunk respectively. Given their size and location patients often consider them cosmetically unacceptable, using the Medlite Nd:Yag laser these birthmarks can be treated effectively with excellent results.

