

We recommend annual skin cancer screenings for almost everyone. Essentially all skin cancer can be cured if detected early, and an annual skin cancer screening is the best way to find them at this early stage. Patients with a skin cancer history usually require screening every 3 to 6 months. Skin cancer screenings are truly life saving! Don’t be shy—make your appointment today! Contact us today to schedule an appointment.
Dr. Robinson offers a full 20-30 minute thorough skin exam. You'll be given a gown and asked to take off everything but your undergarments. The gown and undergarments can be moved in ways to keep areas of your body covered during the exam and to protect your privacy. Your appointment will involve a thorough examination of your skin — from the top of your scalp to the bottoms of your feet — by a board-certified dermatologist. Remove any nail polish, this will allow us to fully examine your fingers, nails, and nail beds. We will look for suspicious spots that could be cancerous.
Warts are non-cancerous skin growths caused by a viral infection in the top layer of the skin. Viruses that cause warts are called human papillomavirus (HPV). There are over 100 different types of HPV and some of these cause warts. Warts in the genital area, genital warts, are sexually transmitted and are considered a sexually transmitted infection (STI). A vaccine is available to help protect against the types of HPV that cause genital warts. Genital warts can increase a person's risk of certain types of cancer, therefore vaccination is recommended to decrease your risk.
There are several different kinds of warts including:
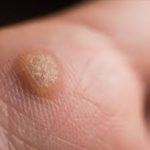
Common warts usually grow on the fingers, around the nails and on the backs of the hands. They are more common where skin has been broken, for example where fingernails are bitten or hangnails picked. These are often called "seed" warts because the blood vessels to the wart produce black dots that look like seeds.
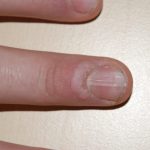
Subungual warts: These warts develop beneath fingernails or toenails. While subungual warts are typically not cancerous, there is a risk of them transforming into a type of skin cancer called squamous cell carcinoma, particularly when caused by high-risk types of HPV. Subungual squamous cell carcinoma can also mimic the appearance of a wart, leading to misdiagnosis and delayed treatment.
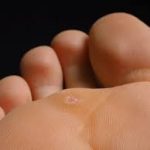
Foot warts usually appear on the soles (plantar area) of the feet and are called plantar warts. When plantar warts grow in clusters they are known as mosaic warts. Most plantar warts do not stick up above the surface like common warts because the pressure of walking flattens them and pushes them back into the skin. Like common warts, these warts may have black dots. Plantar warts are uncomfortable and painful, feeling like a stone in the shoe.
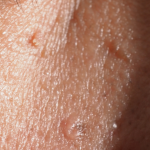
Flat warts appear as small, smooth usually skin colored, pink or brown bumps on the skin. Common places for flat warts are the face, top of the hands, top of the feet, arms, and legs.
Genital warts - warts in the genital area, also called "condyloma acuminatum", are a sexually transmitted infection (STI) caused by a certain type of human papillomavirus (HPV).They appear as small, flesh-colored bumps in the genital area. While treatable, genital warts are a recurring condition and can be spread through skin-to-skin contact during sexual activity. Vaccination against HPV can protect against certain strains that cause genital warts.
To prevent warts from spreading, dermatologists recommend the following:
While you may be able to clear a wart at home, some warts can be stubborn. If the person has a weakened immune system, it can be difficult to get rid of warts. Sometimes, what looks like a wart turns out to be a callus or another type of growth.
A board-certified dermatologist can help by:
Sometimes, warts can be stubborn, so they don’t clear with treatment that you can buy without a prescription. A dermatologist can create an effective treatment plan.
Because warts can spread, cause pain and affect your day-to-day life, your healthcare provider may recommend treatment. Options include:
Vitiligo is a skin condition resulting from the loss of pigment which produces white patches. Any part of the body may be affected. Usually both sides of the body are affected. Common areas of involvement are the face, lips, hands, arms, legs, and genital areas.
Vitiligo affects one or two of every 100 people. About half the people who develop it do so before the age of 20; about 1/5 have a family member with this condition. It may be an autoimmune process (the body makes antibodies to its own pigment cells). Most people with vitiligo are in good general health, although vitiligo may occur with other autoimmune diseases such as thyroid disease
Melanin, the pigment that determines color of skin, hair, and eyes, is produced in cells called melanocytes. If these cells die or cannot form melanin, the skin becomes lighter or completely white
Typical vitiligo shows areas of milky-white skin. However, the degree of pigment loss can vary within each vitiligo patch. There may be different shades of pigment in a patch, or a border of darker skin may circle an area of light skin.
Vitiligo often begins with a rapid loss of pigment. This may continue until, for unknown reasons, the process stops. Cycles of pigment loss, followed by times where the pigment doesn't change, may continue indefinitely.
It is rare for skin pigment in vitiligo patients to return on its own. Some people who believe they no longer have vitiligo actually have lost all their pigment and no longer have patches of contrasting skin color. Although their skin is all one color, they still have vitiligo.
The course and severity of pigment loss differ with each person. Light-skinned people usually notice the contrast between areas of vitiligo and suntanned skin in the summer. Year round, vitiligo is more obvious on people with darker skin. Individuals with severe cases can lose pigment all over the body. There is no way to predict how much pigment an individual will lose.
Sometimes the best treatment for vitiligo is no treatment at all. In fair-skinned individuals, avoiding tanning of normal skin can make areas of vitiligo almost unnoticeable because the (no pigment) white skin, of vitiligo has no natural protection from sun. These areas are easily sunburned, and people with vitiligo have an increased risk to skin cancer. A sunscreen with a SPF of at least 30 should be used on all areas of vitiligo not covered by clothing. Avoid the sun when it is most intense to avoid burns.
Disguising vitiligo with make-up, self-tanning compounds or dyes is a safe, easy way to make it less noticeable. Waterproof cosmetics to match almost all skin colors are available. Stains that dye the skin can be used to color the white patches to more closely match normal skin color. These stains gradually wear off. Self-tanning compounds contain a chemical called dihydroxyacetone that does not need melanocytes to make the skin a tan color. The color from self-tanning creams also slowly wears off. None of these change the disease, but they can improve appearance. Micropigmentation tatooing of small areas may be helpful.
If sunscreens and cover-ups are not satisfactory, your doctor may recommend other treatment. Treatment can be aimed at returning normal pigment (repigmentation) or destroying remaining pigment (depigmentation). None of the repigmentation methods are permanent cures.
Aggressive treatment is generally not used in children. Sunscreen and cover-up measures are usually the best treatments. Topical corticosteroids can also be used, but must be monitored. PUVA, an ulta-violet therapy, is usually not recommended until after age 12, and then the risks and benefits of this treatment must be carefully weighed.
Topical Corticosteroids — Creams containing corticosteroid compounds can be effective in returning pigment to small areas of vitiligo. These can be used along with other treatments. These agents can thin the skin or even cause stretch marks in certain areas. They should be used under your dermatologist's care.
PUVA is a form of repigmentation therapy where a type of medication known as psoralen is used. This chemical makes the skin very sensitive to light. Then the skin is treated with a special type of ultraviolet light call UVA. Sometimes, when vitiligo is limited to a few small areas, psoralens can be applied to the vitiligo areas before UVA treatments. Usually, however, psoralens are given in pill form. Treatment with PUVA has a 50 to 70% chance of returning color on the face, trunk, and upper arms and upper legs. Hands and feet respond very poorly. Usually at least a year of twice weekly treatments are required. PUVA must be given under close supervision by your dermatologist. Side effects of PUVA include sunburn-type reactions. When used long-term, freckling of the skin may result and there is an increased risk of skin cancer. Because psoralens also make the eyes more sensitive to light, UVA blocking eyeglasses must be worn from the time of exposure to psoralen until sunset that day to prevent an increased risk of cataracts. PUVA is not usually used in children under the age of 12, in pregnant or breast feeding women, or in individuals with certain medical conditions.
This is a form of phototherapy that requires the skin to be treated two, sometimes three, times a week for a few months. At this time this form of treatment is not widely available. It may be especially useful in treating children with vitiligo.
Transfer of skin from normal to white areas is a treatment available only in certain areas of the country and is useful for only a small group of vitiligo patients. It does not generally result in total return of pigment in treated areas.
Other treatment options include a new topical class of drugs called immunomodulators. Due to their safety profile they may be useful in treating eyelids and children. Excimer lasers may be tried as well.
For some patients with extensive involvement, the most practical treatment for vitiligo is to remove remaining pigment from normal skin and make the whole body an even white color. This is done with a chemical called monobenzylether of hydroquinone. This therapy takes about a year to complete. The pigment removal is permanent.
At this time, the exact cause of vitiligo is not known, however, there may be an inherited component. Although treatment is available, there is no single cure. Research is ongoing in vitiligo and it is hoped that new treatments will be developed.
Time To Smile Again ... A venous lake is a benign, soft, compressible blue bump usually found on or around the lips caused by a dilated vein. While it is benign it can be cosmetically unsightly. With the use of the Nd:YAG laser a venous lake can be treated within seconds and resolved without scarring.
What To Expect:
FAQ's:
Is It Safe? The Nd:YAG laser is clinically proven to be both safe and effective.
How Does It Work? Treatments target the blood in the venous Lake lesion, causing it to regress.
Is The Treatment Suitable For Me? This procedure can be used on all skin types and treatment is suitable for most people. However, prior to treatment please review our cosmetic reimbursement policy.
Urticaria, also known as hives, are localized, pale, itchy, pink wheals (swellings) that can burn or sting. They may occur singularly or in groups on any part of the skin. They are part of an allergic reaction and are very common. Approximately 10-20 percent of the population will have at least one episode in their lifetime. Most episodes of hives disappear quickly in a few days to a few weeks. Occasionally, a person will have them for many months or years. New hives may develop as old ones fade. Hives can vary in size from as small as a pencil eraser to as large as a dinner plate, and may join to form even larger swellings.
Hives are produced by blood plasma leaking through tiny gaps between the cell lining small blood vessels in the skin. Histamine is a chemical released from cells in the skin called mast cells; which lie along blood vessels. Allergic reactions, chemicals in foods, or medications may cause hives; sometimes it is impossible to find out the cause. When hives form around the eyes, lips, or genitals, the tissue may swell excessively. Although frightening, the swelling usually goes away in less than 24 hours. Severe cases of hives may cause difficulty in breathing or swallowing and emergency room care is required.
Acute urticaria lasts less than six weeks. An underlying cause can be frequently identified and eliminated. The most common causes for acute urticaria are foods, drugs, or infections. Insect bites, internal diseases, pressure, cold, or sunlight also may be responsible.
The most common foods that cause urticaria are: nuts, chocolate, shellfish, tomatoes, eggs, berries, and milk. Fresh foods cause hives more often than cooked foods. Food additives and preservatives may also cause hives.
Hives may appear within minutes to several hours after eating, depending upon the site within the digestive tract where the food is absorbed.
Almost any medication -- prescription or over-the-counter -- can cause hives. Antibiotics, pain medications, sedatives, tranquilizers, diuretics (water pills), diet supplements, antacids, arthritis medication, vitamins, herbal supplements, eye and eardrops, laxatives, vaginal douches, or any other non-prescription item can be a potential cause of urticaria. It is important to inform the dermatologist of ALL prescription and over-the-counter medications being used to help find the cause of the hives.
Many infections can cause urticaria. Viral upper-respiratory tract infections (colds) are a comon cause in children. Other viruses, including hepatitis and a number of bacterial and fungal infections, may cause urticaria.
Chronic urticaria lasts more than six weeks. The cause of chronic urticaria is more difficult to identify and is found only in a small percentage of patients. The dermatologist reviews a patient's medical history, asks extensive questions, and conducts a thorough physical examination. Testing, such as blood work or a biopsy, may be necessary.
Physical urticaria may be caused by sunlight, heat, cold, water, pressure, vibration, or exercise. Solar urticaria forms within minutes of sun exposure and typically fades within one to two hours. Cold urticaria appears when the skin is warmed after exposure to cold. Urticaria, which forms in response to the cold or the water when swimming, for example, can produce wheezing, flushing, generalized hives, and fainting.
Dermatographic urticaria forms after firmly stroking or scratching the skin, and can often occur with other forms of urticaria. It affects about five percent of the population. Most people with this condition are otherwise healthy. Dermatographism may last for months or even years.
The best treatment for urticaria is to find and eliminate the cause whenever possible. Antihistamines are prescribed to provide relief and work best if taken on a regular schedule to prevent hives from forming. There are many antihistamines available. No one antihistamine works for everyone. The dermatologist may use combinations to control the urticaria. In severe cases, an injection of epinephrine (adrenalin) may be needed. Cortisone may also bring dramatic relief, but its use must be limited to short periods of time.
Tinea versicolor is a common skin condition due to overgrowth of a skin surface yeast. This overgrowth results in uneven skin color and scaling that can be unsightly and sometimes itch. The yeast normally lives in the pores of the skin and thrives in oily areas such as the neck, upper chest, and back. Tinea versicolor has small, scaly white-to-pink or tan-to-dark spots which can be scattered over the upper arms, chest and back. They may sometimes appear on the neck and the face. On light skin, Tinea versicolor may be faint or can appear as tan-to-pink spots, while on dark skin Tinea versicolor may be light or dark. The fungus grows slowly and prevents the skin from tanning normally. As the rest of the skin tans in the sun, the pale spots, which are affected by the yeast, become more noticeable, especially on dark skin.
Tinea versicolor has small, scaly white-to-pink or tan-to-dark spots which can be scattered over the upper arms, chest and back. They may sometimes appear on the neck and the face. On light skin, Tinea versicolor may be faint or can appear as tan-to-pink spots, while on dark skin Tinea Versicolor may be light or dark. The fungus grows slowly and prevents the skin from tanning normally.
Tinea Versicolor usually produces few symptoms. Occasionally, there is some slight itching that is more intense when a person gets hot.
Most people get tinea versicolor when they are teenagers or young adults. It is rare in the elderly and children, except in tropical climates where it can occur at any age. Both dark and light skinned people are equally prone to its development. People with oily skin may be more susceptible than those with naturally dry skin.
The yeast is normally present in small numbers on everyone's skin. Anyone can develop an overgrowth of yeast. During the summer months when the temperature and humidity are high, the yeast can increase. The excess yeast on the skin prevents the normal pigmentation process, resulting in light and dark spots. In tropical countries with continuous high heat and high humidity, people can have these spots year round. In other climates, the spots generally fade in the cooler and drier months of the year. Why some people get tinea versicolor and others do not is unclear.
In tropical countries with continuous high heat and high humidity, people can have these spots year round. In other climates, the spots generally fade in the cooler and drier months of the year.
Although the light or dark colored spots can resemble other skin conditions, tinea versicolor can be easily recognized by a dermatologist. In most cases, the appearance of the skin is diagnostic, but a simple examination of the fine scales scraped from the skin can confirm the diagnosis. Scales are lightly scraped onto a slide and examined under a microscope for the presence of the yeast. A special light may help to make the diagnosis by showing a yellow green color where the skin is affected.
Tinea versicolor is treated with topical or oral medications. Topical treatment includes special cleansers including some shampoos, creams, or lotions applied directly to the skin.
Several oral medications have been used successfully to treat tinea versicolor. Because of possible side effects, or interactions with other medications, the use of these prescription medicines should be supervised by a dermatologist. After any form of treatment, the uneven color of the skin may remain for several months after the yeast has been eliminated until the skin repigments normally.
Tinea versicolor may recur. Special cleansers may decrease episodes when used once or twice a month, especially during warm humid months of the year.
Each patient is treated by the dermatologist according to the severity and location of the disease, the climate, and the desire of the patient. It's important to remember that the yeast is easy to kill, but it can take weeks or months for the skin to regain its normal color.
Telangectasias (commonly known as spider veins) are dilated or broken blood vessels located near the surface of the skin. They often occur on the face and particularly on the sides of the nose. They often look like small red or pink lines, which temporarily whiten when pressed.
Some Symptoms Of Spider Veins Include:
Common Causes of Spider Veins
Spider veins are generally caused by weak or damaged valves. The following causes can contribute to weaker blood flow in certain areas of your body.
Treatment(s):
Thankfully, laser therapy is safe and efficacious treatment. It is an easy in-office treatment that can be performed during ones lunch break. In 10 minutes those red lines are gone and you can go right back to work. No wound care or dressings needed.
Sclerotherapy is also a treatment option. A special solution is injected directly into the affected veins, forcing the veins to close and the blood to redirect into healthier veins. The old vein turns into scar tissue that your body will eventually absorb, causing it to fade.

It is important to treat a sunburn as soon as you notice it.
The first thing you should do if you feel you have or are getting a sunburn is get out of the sun, preferably go indoors. Once indoors, these tips can help relieve the discomfort:
If you have fever, chills, headache or any questions about your sunburn please call our office to schedule an appointment. Although it may seem like a temporary condition, sunburn is a result of skin receiving too much exposure from the sun’s ultraviolet (UV) rays and can cause long-lasting damage to the skin. This damage increases a person’s risk for getting skin cancer.
Squamous cell carcinoma is the second most common cancer of the skin. More than 250,000 new squamous cell carcinomas are diagnosed every year in the United States. Middle-aged and elderly people, especially those with fair complexions and frequent sun exposure, are most likely to be affected.
The cancer develops in the outer layer of the skin (the epithelium). Some squamous cell carcinomas arise from small sandpaper-like lesions called solar (sun) or actinic keratosis. It is possible for squamous cell carcinoma to spread to other areas of the body; therefore, early treatment is important.
Squamous cell carcinomas usually appear as crusted or scaly patches on the skin with a red, inflamed base, a growing tumor, or a non-healing ulcer. They are generally found in sun-exposed areas like the face, neck, arms, scalp, backs of the hands, and ears. The cancer also can occur on the lips, inside the mouth, on the genitalia, or anywhere on the body. Any lesion, especially those that do not heal, grow, bleed, or change in appearance, should be evaluated by a dermatologist.
Ultraviolet light exposure (from the sun or indoor tanning devices) greatly increases the chance of developing skin cancer. Although anyone can get squamous cell carcinoma, people with light skin who sunburn easily are at the highest risk. The chance of developing skin cancer increases with age and a history of severe sunburns as a child. Many less common skin conditions, organ transplantation, chronic skin ulcers, prior x-ray treatment (e.g., for acne in the 1950s), arsenic ingestion, smoking, and toxic exposure to tars and oils can predispose individuals to the development of squamous cell carcinoma.
These skin cancers are usually locally destructive. If left untreated, squamous cell carcinoma can destroy much of the tissue surrounding the tumor and may result in the loss of a nose or ear, for example. Aggressive types of squamous cell carcinomas, especially those on the lips and ears, or untreated cancers, can spread to the lymph nodes and other organs resulting in approximately 2,500 deaths each year in the United States.
A skin biopsy for microscopic examination may be done to confirm the diagnosis. A variety of different treatment options can be used depending on the location of the tumor, size, microscopic characteristics, health of the patient, and other factors. Most therapies are relatively minor office-based procedures that require only local anesthesia. Surgical excision to remove the entire cancer is the most commonly used treatment. "Mohs" micrographic controlled surgery, a method which requires specialized training by dermatologic surgeons, can be used to remove the tumor while sparing as much normal skin as possible. Other dermatologic surgical procedures include laser surgery, cryosurgery (liquid nitrogen - the frozen method), radiation therapy, and electrodesiccation and curettage which involves alternately scraping and cauterizing (burning) the tumor with low levels of electricity.
Spider Veins are very small veins caused by a dilation of the small venules under the skin. This occurs when the pressure inside the vein increases enough to overcome normal resistance of the vein wall. The ability of veins to resist increased pressure is reduced with hormonal changes.
Reticular Veins are small, bluish-colored veins that carry blood to the skin venules and are larger than spider veins. These veins have thin walls and dilate with excessive venous pressure. When this occurs, they become large enough to be unsightly, but are not considered to be varicose veins.
In recent years medical lasers have made great advancements in sophistication. Today, lasers are safely used for a wide variety of cosmetic non-invasive treatments. Laser Therapy treatment is extremely safe and effective on leg veins, as well as veins visible on the face, neck, and chest. Laser treatment also corrects benign pigmented lesions such as age spots and birthmarks. These non-invasive treatments are increasingly popular because they have very few side effects, and one can resume regular activities immediately following treatment.
Both men and women, light and dark-skinned individuals can now safely and effectively benefit from laser therapy for spider veins. Patients using blood thinners or afflicted with a serious illness generally are not candidates for treatment. Patients with dark suntans or photosensitivity disorders, uncontrolled or severe diabetes, bleeding disorders, or those currently taking photosensitizing medications may also be restricted from candidacy.
The number of treatments necessary to resolve your vein concerns depends on the size of the vein and your body's ability to heal. During your consultation, you will be given an estimate of the number of treatments required to obtain optimal results.
Treatment may vary from 15 to 30 minutes. As a result of treatment, the walls of the veins are damaged by the laser's heat. The body next induces a healing process. The veins shrink and become less visible or disappear altogether. Medical studies have documented exceptional results on veins with laser treatments.
The beauty of this treatment is that there is no down time involved. You can resume most of your regular activities immediately. Your doctor may use various methods to reduce the pain that may be associated with this procedure. Swelling and mild bruising can occur, but almost always resolve over a short period of time. Limiting sun exposure, avoiding strenuous exercise, and wearing compression stockings will greatly minimize the risk of complications immediately following your treatment.
Laser Therapy treats many types of leg veins, including shallow spider veins and reticular veins.
Spider Veins are very small veins caused by a dilation of the small venules under the skin. This occurs when the pressure inside the vein increases enough to overcome normal resistance of the vein wall. The ability of veins to resist increased pressure is reduced with hormonal changes.
Reticular Veins are small, bluish-colored veins that carry blood to the skin venules and are larger than spider veins. These veins have thin walls and dilate with excessive venous pressure. When this occurs, they become large enough to be unsightly, but are not considered to be varicose veins.
Schedule an office visit to discuss your concerns and skincare goals with Dr. Robinson and the office visit cost will be applied to the future cost for the "consulted procedure". The "consulted procedure" must be completed within 30 days of your consult visit.

