

Hair loss is one of the most common disorders that dermatologists diagnose and treat, the medical term for hair loss is alopecia. Treatment for hair loss is most effective when started early.
To pinpoint the cause of your hair loss, Dr. Robinson begins by gathering information, by asking questions, looking closely at your scalp, nails, any other area with hair loss and by testing the health of your hair. We lose our hair for many (with emphasis on many) reasons.
With so many causes, it can be challenging to figure out why your hair is falling out. If you want to do something about it, though, knowing the cause is important. In many cases, hair loss can be successfully treated, or action taken to prevent further hair loss. The key to getting results is knowing the true cause of your hair loss.
Dr. Robinson specializes in treating the skin, hair, and nails. He has the expertise and tools to help get to the root cause of a person’s hair loss.
The sooner you find the cause, the better your outcome. The less hair you lose, the more successful treatment (or prevention) tends to be.
Some products are effective. Minoxidil (Rogaine®) can safely and effectively treat a few causes of hair loss. People who have hereditary hair loss can have some regrowth with this product. Using an at-home laser can also be part of an effective treatment plan for someone who has hereditary hair loss.
Again, the key to getting results is to know the cause.
Yes, it’s normal to lose between 50 and 100 hairs a day. That’s because our bodies continually grow new hair and shed old hair. This shedding is not a sign of hair loss.
A receding hairline, bald spot, or overall thinning is a sign of hair loss
Hair loss has many causes. What’s causing your hair loss can determine whether your hair:
Both men and women develop this type of hair loss, which is the most common cause of hair loss worldwide. In men, it’s called male pattern hair loss. Women get female pattern hair loss. Regardless of whether it develops in a man or women, the medical term is androgenic alopecia.
No matter which term you use, it means that you’ve inherited genes that cause your hair follicles (what each hair grows out of) to shrink and eventually stop growing hair. Shrinking can begin as early as your teens, but it usually starts later in life.
In women, the first noticeable sign of hereditary hair loss is usually overall thinning or a widening part.
When a man has hereditary hair loss, the first sign is often a receding hairline or bald spot at the top of his head.
Is regrowth possible?
Yes, treatment can help stop or slow hair loss. It may also help regrow hair. The earlier treatment is started, the better it works. Without treatment, you will continue to lose hair.
With age, most people notice some hair loss because hair growth slows. At some point, hair follicles stop growing hair, which causes the hair on our scalp to thin. Hair also starts to lose its color. A woman’s hairline naturally starts to recede.
Alopecia areata is a disease that develops when the body’s immune system attacks hair follicles (what holds the hair in place), causing hair loss. You can lose hair anywhere on your body, including your scalp, inside your nose, and in your ears. Some people lose their eyelashes or eyebrows.
Is regrowth possible?
Yes. If your hair fails to grow back on its own, treatment may help stimulate regrowth.
If you receive chemotherapy or have radiation treatment to your head or neck, you may lose all (or most of) your hair within a few weeks of starting treatment.
Is regrowth possible?
Hair usually starts to regrow within months of finishing chemotherapy or radiation treatments to the head or neck. Dermatologists can offer medication to help hair grow back more quickly.
Is it preventable?
Wearing a cooling cap before, during, and after each chemotherapy session may help prevent hair loss.
A few months after giving birth, recovering from an illness, or having an operation, you may notice a lot more hairs in your brush or on your pillow. This can also happen after a stressful time in your life, such as a divorce or death of a loved one.
Is regrowth possible?
If the stress stops, your body will readjust and the excessive shedding will stop. When the shedding stops, most people see their hair regain its normal fullness within 6 to 9 months.
If you color, perm, or relax your hair, you could be damaging your hair. Over time, this damage can lead to hair loss.
Is regrowth possible?
You can change how you care for your hair, which can prevent hair loss. Once you damage a hair follicle, hair cannot grow from that follicle. Having many damaged hair follicles creates permanent bald spots.
If you often wear your hair tightly pulled back, the continual pulling can lead to permanent hair loss. The medical name for this condition is traction alopecia.
Is regrowth possible?
No. You can prevent hair loss by making some changes.
A common cause of this imbalance is polycystic ovary syndrome (PCOS). It leads to cysts on a woman’s ovaries, along with other signs and symptoms, which can include hair loss. Stopping some types of birth control pills can cause a temporary hormonal imbalance. Women who develop a hormonal imbalance can develop thinning hair (or hair loss) on their scalp.
Is regrowth possible?
Treatment may help.
A scalp infection can lead to scaly and sometimes inflamed areas on your scalp. You may see what look like small black dots on your scalp. These are actually stubs of hair. Some people develop a bald spot.
Is regrowth possible?
Yes, treatment can get rid of the infection. Once the infection clears, hair tends to grow.
A possible side effect of some medications is hair loss. If you think a medication is causing your hair loss, ask the doctor who prescribed it if hair loss is a possible side effect. It’s essential that you do not stop taking the medication before talking with your doctor. Abruptly stopping some medications can cause serious health problems.
Is regrowth possible?
Yes.
Many people who have plaque psoriasis develop psoriasis on their scalp at some point. This can lead to hair loss.
Is regrowth possible?
Hair tends to regrow once the scalp psoriasis clears, but this takes time
If you have a problem with your thyroid, you may see thinning hair. Some people notice that their hair comes out in clumps when they brush it.
Is regrowth possible?
Yes, treating the thyroid disease can reverse the hair loss.
While your hair may regrow on its own, our practice may recommend treatment to help it grow more quickly. Sometimes, treatment is essential to prevent further hair loss.
Oral Minoxidil is by prescription only. Dermatologists began using low-dose oral minoxidil for hair loss after noticing the side effects of the high-dose version of the drug used to treat high blood pressure increased hair growth. The efficacy of 5mg oral minoxidil for men with androgenetic alopecia was tested. Researchers concluded that 43% of the patients had excellent results in hair growth. Typically, people prefer oral to topical. They find it easier and more convenient to take the medication orally, may be able to save money with an oral minoxidil prescription and prefer not to have residue on their hair.
Topical Minoxidil 5% Solution aka Rogaine solution or foam is available over the counter. Effectiveness of topical Minoxidil works for about 2 out of 3 men. It's most effective if you're under age 40 and have only recently started to lose your hair. How to use it: Twice a day, when your hair is dry, apply minoxidil on your scalp where the hair has started to thin. Minoxidil can help maintain the regrowth after you stop applying the corticosteroid. It has few side effects, so it’s considered a good option for children. New hair growth may appear in about 12 weeks.
Laser for at-home use: You can buy laser caps and laser combs to treat hair loss at home. While only a few studies have looked at these devices, the results are promising.
In one study, more than 200 men and women who had hereditary hair loss were given either a laser hair comb or a sham device that looked like a laser comb. The patients used the device that they were given 3 times per week for 26 weeks.
The researchers found that some patients using the laser rather than the sham device saw overall thicker and fuller hair.
It’s important to understand that not everyone who used a laser saw regrowth.
More studies are needed to find out who is most likely to benefit from this treatment and whether these devices cause long-term side effects.
PRP (platelet-rich plasma) therapy
PRP (platelet-rich plasma) therapy for hair loss is a three-step medical treatment in which a person’s blood is drawn, processed, and then injected into the scalp.
PRP injections trigger natural hair growth and maintain it by increasing blood supply to the hair follicle and increasing the thickness of the hair shaft. Sometimes this approach is combined with other hair loss procedures or medications.
Another treatment option is to take prescription medication. The type of medication prescribed will depend on your:
With any medication, side effects are possible. Ask your dermatologist about possible side effects that you might experience while taking one of these medications to treat hair loss. The medications include:
Finasteride (Propecia®): The U.S. Food and Drug Administration (FDA) approved this medication to treat male pattern hair loss. When taken as directed, finasteride can:
Finasteride is a pill that you take once a day. Taking it at the same time each day seems to produce the best results.
Like other treatments for hair loss, this, too, takes time to work. It usually takes about 4 months to notice any improvement.
Finasteride tends to be more effective if you begin taking it when you first notice hair loss. A dermatologist may also prescribe this medication to treat a woman who has hereditary hair loss and cannot get pregnant.
If finasteride works for you, you will need to keep taking it to continue getting results. Once you stop, you’ll start losing hair again. Before taking this medication, be sure to discuss possible side effects with your prescribing doctor.
Spironolactone: For women who have female pattern hair loss, this medication may be an option. It can:
Studies indicate that this medication is effective in about 40% for women who have female pattern hair loss. In one study of 166 women taking spironolactone, 42% said they had mild improvement, and 31% reported increased thickness.
It’s essential that you not become pregnant while taking spironolactone. This medication can cause birth defects. To prevent pregnancy, Dr. Robinson will also prescribe a birth control pill if it’s possible for you to get pregnant.
If your blood test reveals that you’re not getting enough biotin, iron, or zinc, Dr. Robinson may recommend taking a supplement. If you’re not getting enough protein, he can tell you how to boost your intake.
You should only take biotin, iron, or zinc when your blood test shows that you have a deficiency. If your levels are normal, taking a supplement can be harmful. For example, if you take too much iron, you can develop iron poisoning. Early signs of this include stomach pain and vomiting.
Other supplements meant to help with hair loss tend to contain a lot of one nutrient. Because this can cause you to get too much of the nutrient, we may recommend taking a multivitamin instead.
Do you feel uncomfortable taking medication? Does your schedule limit the amount of time you have for treatment? Is the cost of treatment, which insurance generally will not cover, too expensive?
If you answered yes to any of these questions, we may recommend a wig or concealer.
While these cannot slow hair loss or help you regrow hair, they can boost your self-esteem. Another advantage is that a wig or concealer offers immediate results.
Many types of wigs, including ones that can be custom-made for you, are available. If you’re looking for a concealer, such as a spray or powder that can hide hair loss, you’ll find many products available online. With endless choices, it can be helpful to have a dermatologist guide you in selecting one.
With an accurate diagnosis, many people who have hair loss can see hair regrowth. If you need treatment for regrowth, the earlier you start, the more likely you are to see regrowth.
It’s important to understand that:
No one hair loss treatment works for everyone. Once Dr. Robinson finds the cause(s), he will tell you whether treatment is recommended. Sometimes, your hair will regrow on its own, making treatment unnecessary.
edit in Oxygen
Measles is an airborne, extremely infectious and potentially severe rash illness. It can be very serious for small children, but is easily preventable by a vaccine. Two doses of MMR vaccine are 97% effective at preventing measles, 1 dose is 93% effective. It is uncommon for someone fully vaccinated to develop measles. However, breakthrough infections (when someone becomes infected after they have been vaccinated) can occur, especially in communities experiencing an outbreak where high levels of measles virus are circulating. But the good news is, fully vaccinated people who get measles seem more likely to have a milder illness. Fully vaccinated people seem also less likely to spread the disease to other people, including people who can’t get vaccinated because they are too young or have weakened immune systems.
Measles was declared eliminated in the United States in 2000. This was thanks to a very high percentage of people receiving the safe and effective measles, mumps, and rubella (MMR) vaccine. In recent years, however: U.S. MMR coverage among kindergarteners is now below the 95% coverage target—much lower in some communities—and is decreasing. The unvaccinated individuals have been protected through community immunity (herd immunity), meaning the vaccinated community.
The disease spreads through the air by respiratory droplets produced from coughing or sneezing or touching an infected surface. The measles virus can linger in the air for several hours after an infected person coughs or sneezes.
Measles is not a seasonal virus. However, measles is often spread over times of high travel (like spring break) or in situations where unvaccinated persons are in close quarters (like summer camp).
Immediately call your healthcare provider and let them know that you have been exposed to someone who has measles. Your healthcare provider can:
Determine if you are immune to measles based on your vaccination record, age, or laboratory evidence.
Make special arrangements to evaluate you, if needed, without putting other patients and medical office staff at risk.
If you are not immune to measles, MMR vaccine or a medicine called immune globulin may help reduce your risk of developing measles. Your healthcare provider can advise you, and monitor you for signs and symptoms of measles.
If you are not immune and do not get MMR or immune globulin, you should stay away from settings where there are susceptible people (such as schools, hospitals, or childcare) until your healthcare provider says it's okay to return. This will help ensure that you do not spread it to others.
Measles symptoms don't appear until 10 to 14 days after exposure. They include:
If you have measles, you should stay home for four days after you develop the rash. Staying home is an important way to not spread measles to other people. Ask your healthcare provider when it is safe to be around other people again.
You should also:
CDC considers you protected from measles if you have written documentation (records) showing at least one of the following:
You received two doses of measles-containing vaccine, and you are:
No. CDC considers people who received two doses of measles vaccine as children according to the U.S. vaccination schedule protected for life, and they do not ever need a booster dose.
If you're not sure whether you are fully vaccinated, talk with your healthcare provider.
There's no treatment to get rid of an established measles infection, but over-the-counter fever reducers or vitamin A may help with symptoms. Measles usually goes away on its own after about 10 to 14 days.
Vaccines, maintenance, and post exposure prophylaxis:
Vaccines, maintenance, and post-exposure prophylaxis
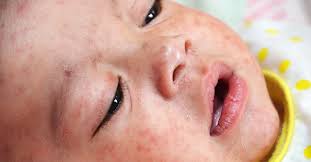
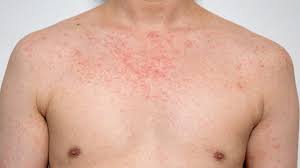
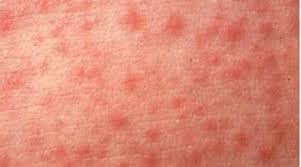
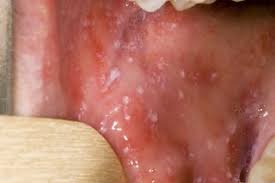
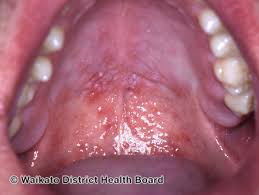
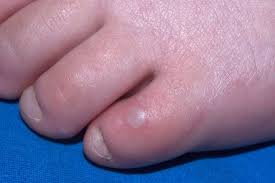
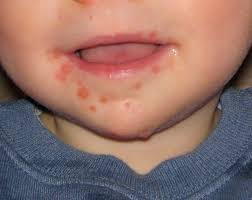
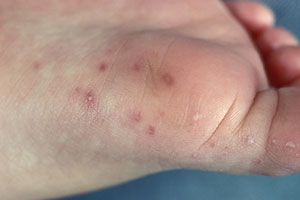
Hand-Foot-Mouth Disease is a mild, contagious viral infection common in young children. It may causes a blister-like rash on your child's hands and feet and painful ogres in their mouth.The disease most often affects babies and children younger than 5 years old. HFMD is typically mild and usually clears up on it's own within 7-10 days.
Hand, foot and mouth disease symptoms typically appear in two stages. When the illness first starts, your child may have flu-like symptoms, such as
After a couple of days, these symptoms will go away and new symptoms will develop:
Viruses belonging to the coxsackievirus and enterovirus families. These viruses can be found in your child's digestive tract, including:
Yes, HFMD is contagious. Your child is most contagious during the first few days of the illness, often before the rash appears. Your child is less likely to spread it to others once the rash/blisters dry up. However, the virus can live in their stool (poop) for weeks after the rash goes away.
Your dermatologist or healthcare provider can diagnose HFMD by looking at your child's blisters. Occasionally, the will test for the virus by sending throat swab samples, or samples taken from blisters or stool (poop) to a lab
If you know your child has been exposed to the virus, alert their provider before scheduling an appointment to protect the health of others. You provider may suggest a virtual visit and make treatment suggestion over the phone.
There is no medication for HFMD. Antibiotics won't work because they don't treat viruses. Fortunately, symptoms are usually mild. Over the counter (OTC) pain relievers such as acetaminophen (Tylenol) and ibuprofen (Advil, Motrin) for fever and pain. Do not give your child aspirin, w which may cause Reye's syndrome.
The viruses that cause Hand, foot and mouth disease are highly contagious. The infection often spreads before a person realizes they're sick. You can slow or stop the spread of the illness through these good hygiene habits.

edit in Oxygen
Advanced skin cancer treatment with no downtime, scarring, or bleeding, better results than MOHS or cold steel excision.
Patients on anticoagulant therapy do not have to stop their medication before treatment, therefore not increasing their risk for stroke and/or heart attack, quick healing, & no risk of post-operative complications!
This treatment is especially great for actors/actresses or professionals in the public eye who can't afford downtime or a scar, athletes or weekend warriors who want to continue their workouts unencumbered and helpful with infirm or older patients who are not able to perform extensive wound care and withstand the rigors of a skin flap or graft.
Non-ablative fractional laser therapy has already demonstrated remarkable success with minimal downtime & discomfort as a gentle yet effective treatment of actinic keratosis (AK), the most common type of pre-cancerous skin conditions.
Now we can add the use of non-ablative fractional laser therapy as the up and coming gold standard to the treatment of squamous and basal cell carcinomas.
Shingles causes a painful, blistering rash on your skin. If you get shingles, you may notice the following three stages:
Before the rash appears: For 1 to 2 days before the rash appears, you may have pain, itching, burning, or tingling on an area of skin where the rash will develop. Some people have described an “electrical sensation” on their skin before getting the rash.
Rash appears: A painful, blistering rash appears or sometimes it can look like a group of hives. It usually appears on one side of your body, often on the torso; however, it can appear anywhere on your skin. Some people get more blisters after the rash appears, so it can seem that the rash is spreading.
Rash starts to clear: As the rash clears, the blisters may open, bleed, and scab over. For most people, the rash will clear within 2 to 4 weeks.
If you have a rash of blisters on your skin or a rash that looks like those shown below, schedule an appointment immediately for a diagnosis. If you have shingles, it’s important to get treatment, preferably within 1 to 3 days. If you’ve had the rash for longer than 2 to 3 days, it’s still important to schedule an appointment!
Along with a painful, blistering rash, some people can also have one or more of the following:
Rash: PLEASE call our office to schedule an appointment immediately or another health-care provider within 3 days of getting the rash. When treatment is started within 3 days, it can prevent possible complications, such as long-lasting nerve pain.
Receiving treatment after 3 days still has its benefits, you should still schedule an appointment!
Before starting treatment, a healthcare provider should confirm the diagnosis of shingles. If shingles is diagnosed, an antiviral medication - such as acyclovir, famciclovir, or valacyclovir, may be prescribed to:
Pain: Over-the-counter medication(s) can help, such as:
If you have severe pain, we may other prescribe a medication that reduces inflammation & provides additional comfort.
Talk with your dermatologist about getting the shingles vaccine, Shingrix. You can get shingles again. A shingles vaccine that the U.S. Food and Drug Administration (FDA) approved in 2017 can greatly reduce your risk of developing shingles again. You can learn more about this vaccine at, Shingles Vaccine, CDC.
The CDC recommends that adults 50 years and older get two doses of the shingles vaccine, Shingrix (recombinant zoster vaccine) to prevent shingles and the complications from the disease. Adults 19 years and older who have weakened immune systems because of disease or therapy should also get two doses of Shingrix, as they have a higher risk of getting shingles and related complications.
Until the shingles rash clears, you are contagious.
Anyone who has NOT had chickenpox (or the vaccine for chickenpox) can catch the virus. An active, untreated Shingles infection can cause chickenpox. Transmission usually happens through direct contact with the fluid from the rash blisters, not through casual contact or the air (unlike primary chickenpox). To avoid infecting others, who could get chickenpox dermatologists recommend that you do the following until the rash clears:
Shingles is caused by reactivation of the chickenpox virus already in your body and usually appears in a localized area. You cannot give someone else shingles, but the virus can spread through direct contact with the rash and cause chickenpox in someone who has never had it or hasn’t been vaccinated.
Pictures of a shingles rash
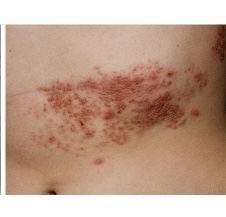
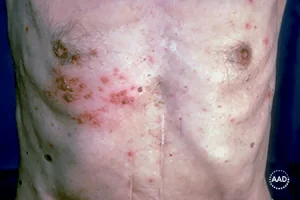
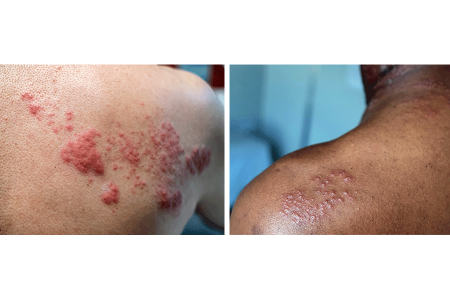
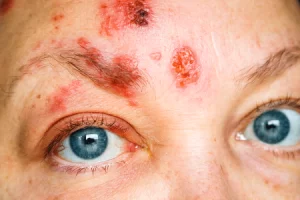
Having a shingles rash on your face is a medical emergency.
Even if the rash isn’t on your eye, it could still affect your eyesight. Immediately seeing a doctor for treatment could save your eyesight.

We are pleased to introduce ProNox™ in our practice, a patient controlled, inhaled analgesia for in-office use. We want our patients to achieve their cosmetic goals worry-free. Patients say that it has made all the difference in moving forward with many cosmetic procedures.
The use of nitrous oxide in Medical, Cosmetic & Laser Dermatologic procedures is becoming more common. Our goal is to provide each patient with a pain-free experience and to work with their varied anxiety levels. While we have excellent topical numbing options for pain control, nitrous oxide can help calm the patient who is nervous or anxious and also help with pain relief.
Dr. Robinson was a pediatric resident @ NYU / NYC Health & Hospitals / Bellevue prior to pursuing dermatology. He enjoys seeing pediatric patients and specializes in difficult to diagnose rashes, birthmarks, acne, warts, molluscum and eczema.

