

Hair loss is one of the most common disorders that dermatologists diagnose and treat, the medical term for hair loss is alopecia. Treatment for hair loss is most effective when started early.
To pinpoint the cause of your hair loss, Dr. Robinson begins by gathering information, by asking questions, looking closely at your scalp, nails, any other area with hair loss and by testing the health of your hair. We lose our hair for many (with emphasis on many) reasons.
With so many causes, it can be challenging to figure out why your hair is falling out. If you want to do something about it, though, knowing the cause is important. In many cases, hair loss can be successfully treated, or action taken to prevent further hair loss. The key to getting results is knowing the true cause of your hair loss.
Dr. Robinson specializes in treating the skin, hair, and nails. He has the expertise and tools to help get to the root cause of a person’s hair loss.
The sooner you find the cause, the better your outcome. The less hair you lose, the more successful treatment (or prevention) tends to be.
Some products are effective. Minoxidil (Rogaine®) can safely and effectively treat a few causes of hair loss. People who have hereditary hair loss can have some regrowth with this product. Using an at-home laser can also be part of an effective treatment plan for someone who has hereditary hair loss.
Again, the key to getting results is to know the cause.
Yes, it’s normal to lose between 50 and 100 hairs a day. That’s because our bodies continually grow new hair and shed old hair. This shedding is not a sign of hair loss.
A receding hairline, bald spot, or overall thinning is a sign of hair loss
Hair loss has many causes. What’s causing your hair loss can determine whether your hair:
Both men and women develop this type of hair loss, which is the most common cause of hair loss worldwide. In men, it’s called male pattern hair loss. Women get female pattern hair loss. Regardless of whether it develops in a man or women, the medical term is androgenic alopecia.
No matter which term you use, it means that you’ve inherited genes that cause your hair follicles (what each hair grows out of) to shrink and eventually stop growing hair. Shrinking can begin as early as your teens, but it usually starts later in life.
In women, the first noticeable sign of hereditary hair loss is usually overall thinning or a widening part.
When a man has hereditary hair loss, the first sign is often a receding hairline or bald spot at the top of his head.
Is regrowth possible?
Yes, treatment can help stop or slow hair loss. It may also help regrow hair. The earlier treatment is started, the better it works. Without treatment, you will continue to lose hair.
With age, most people notice some hair loss because hair growth slows. At some point, hair follicles stop growing hair, which causes the hair on our scalp to thin. Hair also starts to lose its color. A woman’s hairline naturally starts to recede.
Alopecia areata is a disease that develops when the body’s immune system attacks hair follicles (what holds the hair in place), causing hair loss. You can lose hair anywhere on your body, including your scalp, inside your nose, and in your ears. Some people lose their eyelashes or eyebrows.
Is regrowth possible?
Yes. If your hair fails to grow back on its own, treatment may help stimulate regrowth.
If you receive chemotherapy or have radiation treatment to your head or neck, you may lose all (or most of) your hair within a few weeks of starting treatment.
Is regrowth possible?
Hair usually starts to regrow within months of finishing chemotherapy or radiation treatments to the head or neck. Dermatologists can offer medication to help hair grow back more quickly.
Is it preventable?
Wearing a cooling cap before, during, and after each chemotherapy session may help prevent hair loss.
A few months after giving birth, recovering from an illness, or having an operation, you may notice a lot more hairs in your brush or on your pillow. This can also happen after a stressful time in your life, such as a divorce or death of a loved one.
Is regrowth possible?
If the stress stops, your body will readjust and the excessive shedding will stop. When the shedding stops, most people see their hair regain its normal fullness within 6 to 9 months.
If you color, perm, or relax your hair, you could be damaging your hair. Over time, this damage can lead to hair loss.
Is regrowth possible?
You can change how you care for your hair, which can prevent hair loss. Once you damage a hair follicle, hair cannot grow from that follicle. Having many damaged hair follicles creates permanent bald spots.
If you often wear your hair tightly pulled back, the continual pulling can lead to permanent hair loss. The medical name for this condition is traction alopecia.
Is regrowth possible?
No. You can prevent hair loss by making some changes.
A common cause of this imbalance is polycystic ovary syndrome (PCOS). It leads to cysts on a woman’s ovaries, along with other signs and symptoms, which can include hair loss. Stopping some types of birth control pills can cause a temporary hormonal imbalance. Women who develop a hormonal imbalance can develop thinning hair (or hair loss) on their scalp.
Is regrowth possible?
Treatment may help.
A scalp infection can lead to scaly and sometimes inflamed areas on your scalp. You may see what look like small black dots on your scalp. These are actually stubs of hair. Some people develop a bald spot.
Is regrowth possible?
Yes, treatment can get rid of the infection. Once the infection clears, hair tends to grow.
A possible side effect of some medications is hair loss. If you think a medication is causing your hair loss, ask the doctor who prescribed it if hair loss is a possible side effect. It’s essential that you do not stop taking the medication before talking with your doctor. Abruptly stopping some medications can cause serious health problems.
Is regrowth possible?
Yes.
Many people who have plaque psoriasis develop psoriasis on their scalp at some point. This can lead to hair loss.
Is regrowth possible?
Hair tends to regrow once the scalp psoriasis clears, but this takes time
If you have a problem with your thyroid, you may see thinning hair. Some people notice that their hair comes out in clumps when they brush it.
Is regrowth possible?
Yes, treating the thyroid disease can reverse the hair loss.
While your hair may regrow on its own, our practice may recommend treatment to help it grow more quickly. Sometimes, treatment is essential to prevent further hair loss.
Oral Minoxidil is by prescription only. Dermatologists began using low-dose oral minoxidil for hair loss after noticing the side effects of the high-dose version of the drug used to treat high blood pressure increased hair growth. The efficacy of 5mg oral minoxidil for men with androgenetic alopecia was tested. Researchers concluded that 43% of the patients had excellent results in hair growth. Typically, people prefer oral to topical. They find it easier and more convenient to take the medication orally, may be able to save money with an oral minoxidil prescription and prefer not to have residue on their hair.
Topical Minoxidil 5% Solution aka Rogaine solution or foam is available over the counter. Effectiveness of topical Minoxidil works for about 2 out of 3 men. It's most effective if you're under age 40 and have only recently started to lose your hair. How to use it: Twice a day, when your hair is dry, apply minoxidil on your scalp where the hair has started to thin. Minoxidil can help maintain the regrowth after you stop applying the corticosteroid. It has few side effects, so it’s considered a good option for children. New hair growth may appear in about 12 weeks.
Laser for at-home use: You can buy laser caps and laser combs to treat hair loss at home. While only a few studies have looked at these devices, the results are promising.
In one study, more than 200 men and women who had hereditary hair loss were given either a laser hair comb or a sham device that looked like a laser comb. The patients used the device that they were given 3 times per week for 26 weeks.
The researchers found that some patients using the laser rather than the sham device saw overall thicker and fuller hair.
It’s important to understand that not everyone who used a laser saw regrowth.
More studies are needed to find out who is most likely to benefit from this treatment and whether these devices cause long-term side effects.
PRP (platelet-rich plasma) therapy
PRP (platelet-rich plasma) therapy for hair loss is a three-step medical treatment in which a person’s blood is drawn, processed, and then injected into the scalp.
PRP injections trigger natural hair growth and maintain it by increasing blood supply to the hair follicle and increasing the thickness of the hair shaft. Sometimes this approach is combined with other hair loss procedures or medications.
Another treatment option is to take prescription medication. The type of medication prescribed will depend on your:
With any medication, side effects are possible. Ask your dermatologist about possible side effects that you might experience while taking one of these medications to treat hair loss. The medications include:
Finasteride (Propecia®): The U.S. Food and Drug Administration (FDA) approved this medication to treat male pattern hair loss. When taken as directed, finasteride can:
Finasteride is a pill that you take once a day. Taking it at the same time each day seems to produce the best results.
Like other treatments for hair loss, this, too, takes time to work. It usually takes about 4 months to notice any improvement.
Finasteride tends to be more effective if you begin taking it when you first notice hair loss. A dermatologist may also prescribe this medication to treat a woman who has hereditary hair loss and cannot get pregnant.
If finasteride works for you, you will need to keep taking it to continue getting results. Once you stop, you’ll start losing hair again. Before taking this medication, be sure to discuss possible side effects with your prescribing doctor.
Spironolactone: For women who have female pattern hair loss, this medication may be an option. It can:
Studies indicate that this medication is effective in about 40% for women who have female pattern hair loss. In one study of 166 women taking spironolactone, 42% said they had mild improvement, and 31% reported increased thickness.
It’s essential that you not become pregnant while taking spironolactone. This medication can cause birth defects. To prevent pregnancy, Dr. Robinson will also prescribe a birth control pill if it’s possible for you to get pregnant.
If your blood test reveals that you’re not getting enough biotin, iron, or zinc, Dr. Robinson may recommend taking a supplement. If you’re not getting enough protein, he can tell you how to boost your intake.
You should only take biotin, iron, or zinc when your blood test shows that you have a deficiency. If your levels are normal, taking a supplement can be harmful. For example, if you take too much iron, you can develop iron poisoning. Early signs of this include stomach pain and vomiting.
Other supplements meant to help with hair loss tend to contain a lot of one nutrient. Because this can cause you to get too much of the nutrient, we may recommend taking a multivitamin instead.
Do you feel uncomfortable taking medication? Does your schedule limit the amount of time you have for treatment? Is the cost of treatment, which insurance generally will not cover, too expensive?
If you answered yes to any of these questions, we may recommend a wig or concealer.
While these cannot slow hair loss or help you regrow hair, they can boost your self-esteem. Another advantage is that a wig or concealer offers immediate results.
Many types of wigs, including ones that can be custom-made for you, are available. If you’re looking for a concealer, such as a spray or powder that can hide hair loss, you’ll find many products available online. With endless choices, it can be helpful to have a dermatologist guide you in selecting one.
With an accurate diagnosis, many people who have hair loss can see hair regrowth. If you need treatment for regrowth, the earlier you start, the more likely you are to see regrowth.
It’s important to understand that:
No one hair loss treatment works for everyone. Once Dr. Robinson finds the cause(s), he will tell you whether treatment is recommended. Sometimes, your hair will regrow on its own, making treatment unnecessary.
Hyperpigmentation and Melasma affect people of all skin tones and types, often appearing as brown or gray marks on the face and body. These changes in pigmentation can be caused by sun exposure, hormonal shifts, common during pregnancy, inflammation, or even acne. While they’re typically harmless, they can impact your confidence and be difficult to treat without expert guidance. At our practice, we take a customized, science-backed approach to identifying the type of pigmentation and creating a targeted treatment plan that works for your unique skin.
SUN SPOTS:
Also known as liver spots or solar lentigines, sun spots are small, flat brown areas on the skin caused by prolonged exposure to ultraviolet (UV) rays. These spots are marked by an increased number of pigment-producing cells, unlike freckles, which have a normal number of cells that are simply overactive.
Sun spots typically appear on areas that get the most sun exposure, the face, chest, arms, and hands and are especially common in those with lighter skin tones.
Avoiding sun spots completely is nearly impossible. To minimize the risk, we strongly recommend applying a broad-spectrum sunscreen with at least SPF 30, every single day, year-round, regardless of the weather and reapplying every two hours, especially when swimming or sweating.
MELASMA:
Melasma appears as brown patches, most commonly found on the face, especially the cheeks and jawline. It can also show up on the temples and upper lip, where it may resemble a mustache; while it's a common condition, its exact cause remains unclear.
Melasma is influenced by both genetics and hormonal fluctuations. It tends to worsen during times of increased estrogen levels, such as pregnancy or while taking birth control pills. This hormonal link is why melasma is often nicknamed the “mask of pregnancy.” Other contributing factors include heat, ultraviolet (UV) exposure, and blue light from devices like phones, computers, and even indoor lighting.
Melasma is more prevalent in people with melanated skin. For treatment, we recommend using a mix of skin-brightening and lightening products, such as retinoids, antioxidants and hydroquinone. Sunscreen is essential. SPF is non-negotiable, mineral formulas with iron oxides are best, as they also shield against blue light. Even minimal UV exposure can reverse weeks of progress with topical treatments, so daily sunscreen use is critical. There are also in-office procedures, such as peels and lasers, that can help, though it’s important to be treated by a provider who is well versed in treating melasma because it’s easy to exacerbate the condition.
POST-INFLAMMATORY HYPERPIGMENTATION (PIH):
Think of post-inflammatory hyperpigmentation (PIH) as a stain left behind on the skin. Any type of inflammation, whether it’s from a burn, breakout, or other irritation, can leave behind a dark mark in that area. These spots can linger for months or even years, and in some cases, they can be more frustrating than the initial condition itself.
The appearance of PIH varies depending on skin tone. Lighter skin types tend to develop red or pink marks, while deeper skin tones often experience discoloration that’s brown, purple, or even black.
Because PIH (post-inflammatory hyperpigmentation), results from inflammation, we emphasize the importance of treating the root cause first, whether it’s acne, eczema, or another condition. While these dark marks may gradually fade on their own, early intervention often leads to better results.
For quicker results, we recommend targeting hyperpigmentation as soon as it appears, using energy-based treatments tailored to the color of the discoloration.
Lasers use focused light energy to target and break down excess melanin (the pigment responsible for dark spots) in the skin. Your body then gradually clears the pigment particles, resulting in a more even skin tone. We offer a range of advanced laser therapies tailored to the type and depth of discoloration, whether you’re dealing with sun spots, melasma or post-inflammatory hyperpigmentation (PIH) .
Q-switched Nd:YAG Laser: Targets deep pigmentation, including melasma and post-inflammatory hyperpigmentation (PIH), with precision and safety for all skin tones.
Fractional Lasers: These versatile lasers treat pigmentation and improve overall skin quality by stimulating collagen production and resurfacing the skin. Great for PIH (post inflammatory hyperpigmentation), sun damage, acne scarring, uneven tone, and texture.
Each laser treatment is customized to your skin’s needs to ensure safe, effective results. During your consultation, we’ll determine the best approach—often combining laser therapy with topical treatments to maximize improvement and minimize recurrence.
To target brown spots, we use a combination of hydroquinone, kojic acid, vitamin C, and alpha hydroxy acids (AHAs) like glycolic acid. This powerful blend works gently yet effectively to lighten hyperpigmentation while brightening and smoothing the skin. These clinically proven ingredients work synergistically to promote a more even, radiant complexion by visibly reducing dark spots and improving overall skin tone and texture.
We also look for ingredients that inhibit melanin production, such as retinol, which enhances cell turnover, and AHAs, which provide a gentle exfoliating effect to help fade discoloration over time.
Other in-office treatment options include: Glycolic Acid Peels and HydraFacial MD with Brightening Boosters—a targeted super-serum designed to address dullness and uneven texture, even for sensitive skin types.
SHOP HERE: JAS Anti - Aging TRIO, expertly formulated to replenish, exfoliate, and restore your skin’s natural glow. These ingredients work synergistically to visibly brighten, lighten, and tighten the skin for a more even, glowing appearance.
⚠️ Important
Always see a board-certified dermatologist or laser specialist, especially if you have darker skin.
Sun protection is non-negotiable—exposure after treatment can trigger new pigment.
If you are tired of looking older or want the spots removed, schedule a laser consultation and restore your skin to its natural beauty. Our Cosmetic Consultation Reimbursement policy is offered to all patients. Schedule an office visit to discuss your concerns and skincare goals with Dr. Robinson and the office visit cost will be applied to the future cost for the "consulted procedure". The "consulted procedure" must be completed within 30 days of your consult visit.
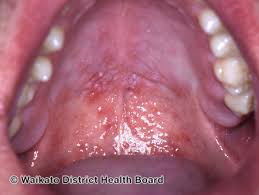
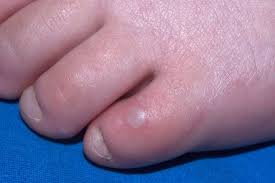
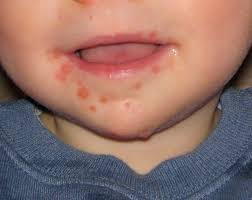
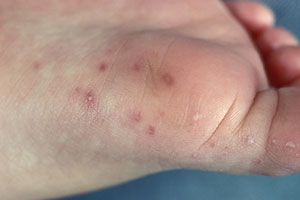
Hand-Foot-Mouth Disease is a mild, contagious viral infection common in young children. It may causes a blister-like rash on your child's hands and feet and painful ogres in their mouth.The disease most often affects babies and children younger than 5 years old. HFMD is typically mild and usually clears up on it's own within 7-10 days.
Hand, foot and mouth disease symptoms typically appear in two stages. When the illness first starts, your child may have flu-like symptoms, such as
After a couple of days, these symptoms will go away and new symptoms will develop:
Viruses belonging to the coxsackievirus and enterovirus families. These viruses can be found in your child's digestive tract, including:
Yes, HFMD is contagious. Your child is most contagious during the first few days of the illness, often before the rash appears. Your child is less likely to spread it to others once the rash/blisters dry up. However, the virus can live in their stool (poop) for weeks after the rash goes away.
Your dermatologist or healthcare provider can diagnose HFMD by looking at your child's blisters. Occasionally, the will test for the virus by sending throat swab samples, or samples taken from blisters or stool (poop) to a lab
If you know your child has been exposed to the virus, alert their provider before scheduling an appointment to protect the health of others. You provider may suggest a virtual visit and make treatment suggestion over the phone.
There is no medication for HFMD. Antibiotics won't work because they don't treat viruses. Fortunately, symptoms are usually mild. Over the counter (OTC) pain relievers such as acetaminophen (Tylenol) and ibuprofen (Advil, Motrin) for fever and pain. Do not give your child aspirin, w which may cause Reye's syndrome.
The viruses that cause Hand, foot and mouth disease are highly contagious. The infection often spreads before a person realizes they're sick. You can slow or stop the spread of the illness through these good hygiene habits.

Wrinkles are caused by the natural aging process, expressions made by muscles and sun damage. Using Sunscreen daily is the Holy Grail Anti-Aging product. Today there are many treatments available to help reduce fine lines and wrinkles on the skin. For deeper creases, a person may require more aggressive technique. With the latest treatments such as Botox, Fillers, Ultherapy, TempSure, and Fraxel laser skin resurfacing, wrinkles can appear less noticeable and even be prevented. These treatments are easy in office procedures that require little to no social downtime. The results can be immediate or seen in just a few weeks. Say "Good-bye" to wrinkles and fine lines and hello to beautiful, younger, smoother looking skin.
Cosmetic Consultation Reimbursement policy offered to all patients. Come discuss your needs and goals with Dr. Robinson and the office visit cost will be applied to future costs for the discussed procedure. Procedure must be completed within 30 days of your consult visit.
Warts are non-cancerous skin growths caused by a viral infection in the top layer of the skin. Viruses that cause warts are called human papillomavirus (HPV). There are over 100 different types of HPV and some of these cause warts. Warts in the genital area, genital warts, are sexually transmitted and are considered a sexually transmitted infection (STI). A vaccine is available to help protect against the types of HPV that cause genital warts. Genital warts can increase a person's risk of certain types of cancer, therefore vaccination is recommended to decrease your risk.
There are several different kinds of warts including:
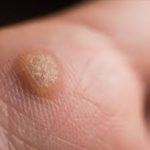
Common warts usually grow on the fingers, around the nails and on the backs of the hands. They are more common where skin has been broken, for example where fingernails are bitten or hangnails picked. These are often called "seed" warts because the blood vessels to the wart produce black dots that look like seeds.
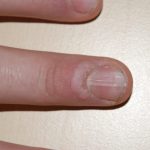
Subungual warts: These warts develop beneath fingernails or toenails. While subungual warts are typically not cancerous, there is a risk of them transforming into a type of skin cancer called squamous cell carcinoma, particularly when caused by high-risk types of HPV. Subungual squamous cell carcinoma can also mimic the appearance of a wart, leading to misdiagnosis and delayed treatment.
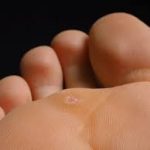
Foot warts usually appear on the soles (plantar area) of the feet and are called plantar warts. When plantar warts grow in clusters they are known as mosaic warts. Most plantar warts do not stick up above the surface like common warts because the pressure of walking flattens them and pushes them back into the skin. Like common warts, these warts may have black dots. Plantar warts are uncomfortable and painful, feeling like a stone in the shoe.
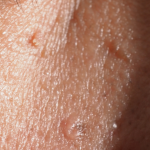
Flat warts appear as small, smooth usually skin colored, pink or brown bumps on the skin. Common places for flat warts are the face, top of the hands, top of the feet, arms, and legs.
Genital warts - warts in the genital area, also called "condyloma acuminatum", are a sexually transmitted infection (STI) caused by a certain type of human papillomavirus (HPV).They appear as small, flesh-colored bumps in the genital area. While treatable, genital warts are a recurring condition and can be spread through skin-to-skin contact during sexual activity. Vaccination against HPV can protect against certain strains that cause genital warts.
To prevent warts from spreading, dermatologists recommend the following:
While you may be able to clear a wart at home, some warts can be stubborn. If the person has a weakened immune system, it can be difficult to get rid of warts. Sometimes, what looks like a wart turns out to be a callus or another type of growth.
A board-certified dermatologist can help by:
Sometimes, warts can be stubborn, so they don’t clear with treatment that you can buy without a prescription. A dermatologist can create an effective treatment plan.
Because warts can spread, cause pain and affect your day-to-day life, your healthcare provider may recommend treatment. Options include:
Vitiligo is a skin condition resulting from the loss of pigment which produces white patches. Any part of the body may be affected. Usually both sides of the body are affected. Common areas of involvement are the face, lips, hands, arms, legs, and genital areas.
Vitiligo affects one or two of every 100 people. About half the people who develop it do so before the age of 20; about 1/5 have a family member with this condition. It may be an autoimmune process (the body makes antibodies to its own pigment cells). Most people with vitiligo are in good general health, although vitiligo may occur with other autoimmune diseases such as thyroid disease
Melanin, the pigment that determines color of skin, hair, and eyes, is produced in cells called melanocytes. If these cells die or cannot form melanin, the skin becomes lighter or completely white
Typical vitiligo shows areas of milky-white skin. However, the degree of pigment loss can vary within each vitiligo patch. There may be different shades of pigment in a patch, or a border of darker skin may circle an area of light skin.
Vitiligo often begins with a rapid loss of pigment. This may continue until, for unknown reasons, the process stops. Cycles of pigment loss, followed by times where the pigment doesn't change, may continue indefinitely.
It is rare for skin pigment in vitiligo patients to return on its own. Some people who believe they no longer have vitiligo actually have lost all their pigment and no longer have patches of contrasting skin color. Although their skin is all one color, they still have vitiligo.
The course and severity of pigment loss differ with each person. Light-skinned people usually notice the contrast between areas of vitiligo and suntanned skin in the summer. Year round, vitiligo is more obvious on people with darker skin. Individuals with severe cases can lose pigment all over the body. There is no way to predict how much pigment an individual will lose.
Sometimes the best treatment for vitiligo is no treatment at all. In fair-skinned individuals, avoiding tanning of normal skin can make areas of vitiligo almost unnoticeable because the (no pigment) white skin, of vitiligo has no natural protection from sun. These areas are easily sunburned, and people with vitiligo have an increased risk to skin cancer. A sunscreen with a SPF of at least 30 should be used on all areas of vitiligo not covered by clothing. Avoid the sun when it is most intense to avoid burns.
Disguising vitiligo with make-up, self-tanning compounds or dyes is a safe, easy way to make it less noticeable. Waterproof cosmetics to match almost all skin colors are available. Stains that dye the skin can be used to color the white patches to more closely match normal skin color. These stains gradually wear off. Self-tanning compounds contain a chemical called dihydroxyacetone that does not need melanocytes to make the skin a tan color. The color from self-tanning creams also slowly wears off. None of these change the disease, but they can improve appearance. Micropigmentation tatooing of small areas may be helpful.
If sunscreens and cover-ups are not satisfactory, your doctor may recommend other treatment. Treatment can be aimed at returning normal pigment (repigmentation) or destroying remaining pigment (depigmentation). None of the repigmentation methods are permanent cures.
Aggressive treatment is generally not used in children. Sunscreen and cover-up measures are usually the best treatments. Topical corticosteroids can also be used, but must be monitored. PUVA, an ulta-violet therapy, is usually not recommended until after age 12, and then the risks and benefits of this treatment must be carefully weighed.
Topical Corticosteroids — Creams containing corticosteroid compounds can be effective in returning pigment to small areas of vitiligo. These can be used along with other treatments. These agents can thin the skin or even cause stretch marks in certain areas. They should be used under your dermatologist's care.
PUVA is a form of repigmentation therapy where a type of medication known as psoralen is used. This chemical makes the skin very sensitive to light. Then the skin is treated with a special type of ultraviolet light call UVA. Sometimes, when vitiligo is limited to a few small areas, psoralens can be applied to the vitiligo areas before UVA treatments. Usually, however, psoralens are given in pill form. Treatment with PUVA has a 50 to 70% chance of returning color on the face, trunk, and upper arms and upper legs. Hands and feet respond very poorly. Usually at least a year of twice weekly treatments are required. PUVA must be given under close supervision by your dermatologist. Side effects of PUVA include sunburn-type reactions. When used long-term, freckling of the skin may result and there is an increased risk of skin cancer. Because psoralens also make the eyes more sensitive to light, UVA blocking eyeglasses must be worn from the time of exposure to psoralen until sunset that day to prevent an increased risk of cataracts. PUVA is not usually used in children under the age of 12, in pregnant or breast feeding women, or in individuals with certain medical conditions.
This is a form of phototherapy that requires the skin to be treated two, sometimes three, times a week for a few months. At this time this form of treatment is not widely available. It may be especially useful in treating children with vitiligo.
Transfer of skin from normal to white areas is a treatment available only in certain areas of the country and is useful for only a small group of vitiligo patients. It does not generally result in total return of pigment in treated areas.
Other treatment options include a new topical class of drugs called immunomodulators. Due to their safety profile they may be useful in treating eyelids and children. Excimer lasers may be tried as well.
For some patients with extensive involvement, the most practical treatment for vitiligo is to remove remaining pigment from normal skin and make the whole body an even white color. This is done with a chemical called monobenzylether of hydroquinone. This therapy takes about a year to complete. The pigment removal is permanent.
At this time, the exact cause of vitiligo is not known, however, there may be an inherited component. Although treatment is available, there is no single cure. Research is ongoing in vitiligo and it is hoped that new treatments will be developed.
Urticaria, also known as hives, are localized, pale, itchy, pink wheals (swellings) that can burn or sting. They may occur singularly or in groups on any part of the skin. They are part of an allergic reaction and are very common. Approximately 10-20 percent of the population will have at least one episode in their lifetime. Most episodes of hives disappear quickly in a few days to a few weeks. Occasionally, a person will have them for many months or years. New hives may develop as old ones fade. Hives can vary in size from as small as a pencil eraser to as large as a dinner plate, and may join to form even larger swellings.
Hives are produced by blood plasma leaking through tiny gaps between the cell lining small blood vessels in the skin. Histamine is a chemical released from cells in the skin called mast cells; which lie along blood vessels. Allergic reactions, chemicals in foods, or medications may cause hives; sometimes it is impossible to find out the cause. When hives form around the eyes, lips, or genitals, the tissue may swell excessively. Although frightening, the swelling usually goes away in less than 24 hours. Severe cases of hives may cause difficulty in breathing or swallowing and emergency room care is required.
Acute urticaria lasts less than six weeks. An underlying cause can be frequently identified and eliminated. The most common causes for acute urticaria are foods, drugs, or infections. Insect bites, internal diseases, pressure, cold, or sunlight also may be responsible.
The most common foods that cause urticaria are: nuts, chocolate, shellfish, tomatoes, eggs, berries, and milk. Fresh foods cause hives more often than cooked foods. Food additives and preservatives may also cause hives.
Hives may appear within minutes to several hours after eating, depending upon the site within the digestive tract where the food is absorbed.
Almost any medication -- prescription or over-the-counter -- can cause hives. Antibiotics, pain medications, sedatives, tranquilizers, diuretics (water pills), diet supplements, antacids, arthritis medication, vitamins, herbal supplements, eye and eardrops, laxatives, vaginal douches, or any other non-prescription item can be a potential cause of urticaria. It is important to inform the dermatologist of ALL prescription and over-the-counter medications being used to help find the cause of the hives.
Many infections can cause urticaria. Viral upper-respiratory tract infections (colds) are a comon cause in children. Other viruses, including hepatitis and a number of bacterial and fungal infections, may cause urticaria.
Chronic urticaria lasts more than six weeks. The cause of chronic urticaria is more difficult to identify and is found only in a small percentage of patients. The dermatologist reviews a patient's medical history, asks extensive questions, and conducts a thorough physical examination. Testing, such as blood work or a biopsy, may be necessary.
Physical urticaria may be caused by sunlight, heat, cold, water, pressure, vibration, or exercise. Solar urticaria forms within minutes of sun exposure and typically fades within one to two hours. Cold urticaria appears when the skin is warmed after exposure to cold. Urticaria, which forms in response to the cold or the water when swimming, for example, can produce wheezing, flushing, generalized hives, and fainting.
Dermatographic urticaria forms after firmly stroking or scratching the skin, and can often occur with other forms of urticaria. It affects about five percent of the population. Most people with this condition are otherwise healthy. Dermatographism may last for months or even years.
The best treatment for urticaria is to find and eliminate the cause whenever possible. Antihistamines are prescribed to provide relief and work best if taken on a regular schedule to prevent hives from forming. There are many antihistamines available. No one antihistamine works for everyone. The dermatologist may use combinations to control the urticaria. In severe cases, an injection of epinephrine (adrenalin) may be needed. Cortisone may also bring dramatic relief, but its use must be limited to short periods of time.
Tinea versicolor is a common skin condition due to overgrowth of a skin surface yeast. This overgrowth results in uneven skin color and scaling that can be unsightly and sometimes itch. The yeast normally lives in the pores of the skin and thrives in oily areas such as the neck, upper chest, and back. Tinea versicolor has small, scaly white-to-pink or tan-to-dark spots which can be scattered over the upper arms, chest and back. They may sometimes appear on the neck and the face. On light skin, Tinea versicolor may be faint or can appear as tan-to-pink spots, while on dark skin Tinea versicolor may be light or dark. The fungus grows slowly and prevents the skin from tanning normally. As the rest of the skin tans in the sun, the pale spots, which are affected by the yeast, become more noticeable, especially on dark skin.
Tinea versicolor has small, scaly white-to-pink or tan-to-dark spots which can be scattered over the upper arms, chest and back. They may sometimes appear on the neck and the face. On light skin, Tinea versicolor may be faint or can appear as tan-to-pink spots, while on dark skin Tinea Versicolor may be light or dark. The fungus grows slowly and prevents the skin from tanning normally.
Tinea Versicolor usually produces few symptoms. Occasionally, there is some slight itching that is more intense when a person gets hot.
Most people get tinea versicolor when they are teenagers or young adults. It is rare in the elderly and children, except in tropical climates where it can occur at any age. Both dark and light skinned people are equally prone to its development. People with oily skin may be more susceptible than those with naturally dry skin.
The yeast is normally present in small numbers on everyone's skin. Anyone can develop an overgrowth of yeast. During the summer months when the temperature and humidity are high, the yeast can increase. The excess yeast on the skin prevents the normal pigmentation process, resulting in light and dark spots. In tropical countries with continuous high heat and high humidity, people can have these spots year round. In other climates, the spots generally fade in the cooler and drier months of the year. Why some people get tinea versicolor and others do not is unclear.
In tropical countries with continuous high heat and high humidity, people can have these spots year round. In other climates, the spots generally fade in the cooler and drier months of the year.
Although the light or dark colored spots can resemble other skin conditions, tinea versicolor can be easily recognized by a dermatologist. In most cases, the appearance of the skin is diagnostic, but a simple examination of the fine scales scraped from the skin can confirm the diagnosis. Scales are lightly scraped onto a slide and examined under a microscope for the presence of the yeast. A special light may help to make the diagnosis by showing a yellow green color where the skin is affected.
Tinea versicolor is treated with topical or oral medications. Topical treatment includes special cleansers including some shampoos, creams, or lotions applied directly to the skin.
Several oral medications have been used successfully to treat tinea versicolor. Because of possible side effects, or interactions with other medications, the use of these prescription medicines should be supervised by a dermatologist. After any form of treatment, the uneven color of the skin may remain for several months after the yeast has been eliminated until the skin repigments normally.
Tinea versicolor may recur. Special cleansers may decrease episodes when used once or twice a month, especially during warm humid months of the year.
Each patient is treated by the dermatologist according to the severity and location of the disease, the climate, and the desire of the patient. It's important to remember that the yeast is easy to kill, but it can take weeks or months for the skin to regain its normal color.
Telangectasias (commonly known as spider veins) are dilated or broken blood vessels located near the surface of the skin. They often occur on the face and particularly on the sides of the nose. They often look like small red or pink lines, which temporarily whiten when pressed.
Some Symptoms Of Spider Veins Include:
Common Causes of Spider Veins
Spider veins are generally caused by weak or damaged valves. The following causes can contribute to weaker blood flow in certain areas of your body.
Treatment(s):
Thankfully, laser therapy is safe and efficacious treatment. It is an easy in-office treatment that can be performed during ones lunch break. In 10 minutes those red lines are gone and you can go right back to work. No wound care or dressings needed.
Sclerotherapy is also a treatment option. A special solution is injected directly into the affected veins, forcing the veins to close and the blood to redirect into healthier veins. The old vein turns into scar tissue that your body will eventually absorb, causing it to fade.

It is important to treat a sunburn as soon as you notice it.
The first thing you should do if you feel you have or are getting a sunburn is get out of the sun, preferably go indoors. Once indoors, these tips can help relieve the discomfort:
If you have fever, chills, headache or any questions about your sunburn please call our office to schedule an appointment. Although it may seem like a temporary condition, sunburn is a result of skin receiving too much exposure from the sun’s ultraviolet (UV) rays and can cause long-lasting damage to the skin. This damage increases a person’s risk for getting skin cancer.

